Section Branding
Header Content
DRC is seeing its worst mpox outbreak — but has no vaccines or treatments yet. Why?
Primary Content
In the Democratic Republic of Congo, the fight against mpox – previously known as monkeypox – is entering a new phase.
While many are anxious to contain the outbreak – the largest mpox outbreak ever recorded in the DRC with more than 4,500 cases so far this year – experts say that's not yet possible: There are no vaccines or treatments in the country right now, and even the testing capacity is severely limited. Instead, this new phase of the mpox fight involves simply getting a better understanding of what exactly is going on.
"We've been doing a lot of groundwork and building support and trying to strengthen things. And now, I hope, we're at a pivot point," says Dr. Jennifer McQuiston of the U.S. Centers for Disease Control and Prevention. "Over the next three weeks, we expect to learn a lot about what's happening on the ground."
The CDC has worked with the DRC for 15 years but has increased their efforts in response to the current mpox outbreak, as has the World Health Organization. They've helped the DRC expand its testing capacity by opening labs in some of the most affected, remote areas. The CDC has also helped fund local epidemiological teams that can provide a more granular understanding of mpox cases.
A changing virus
The DRC's mpox outbreak is noteworthy not only for its size but for the changing nature of the virus.
According to Africa CDC, 11 African countries have reported mpox cases but the DRC is the clear epicenter, with a caseload three times what it was this time last year. The virus, which usually jumps from a small animal to a human and then spreads between people, causes painful lesions and sometimes fever, malaise and even death.
The concern is heightened because the type of mpox circulating, called Clade I, is 10 times deadlier than the type of mpox that caused a worldwide outbreak in 2022. About 10% of Clade I cases are fatal; DRC has confirmed 311 mpox deaths this year. In addition, early evidence suggests there is a new strain of the mpox virus in the eastern part of the DRC that's circulating among sex workers and seems to be sexually transmitted. Clade I has never been known to transmit sexually.
Other countries and international organizations have been working to balance their desire for quick action against the DRC's right to address its own health plans and priorities. The nation is juggling a number of pressing health challenges, including measles, cholera and plague.
"We have work to do," says Dr. Mandy Cohen, the director of the CDC. "[We] have to work with a sovereign country. And they have a lot of health threats... And so helping them work through not just mpox but their overall response is really what we're trying to do."
Earlier this month, the Africa Centres for Disease Control and Prevention – the public health agency of the African Union – helped convene a high-level emergency meeting on mpox in Kinshasa, DRC. The meeting brought together hundreds of experts.
No vaccines in DRC yet
By the end of the meeting, the DRC had announced its intent to use vaccines against mpox – although it still needs to approve the vaccines and draw up a strategy for delivery. In addition, the DRC said it would work quickly to approve a treatment option.
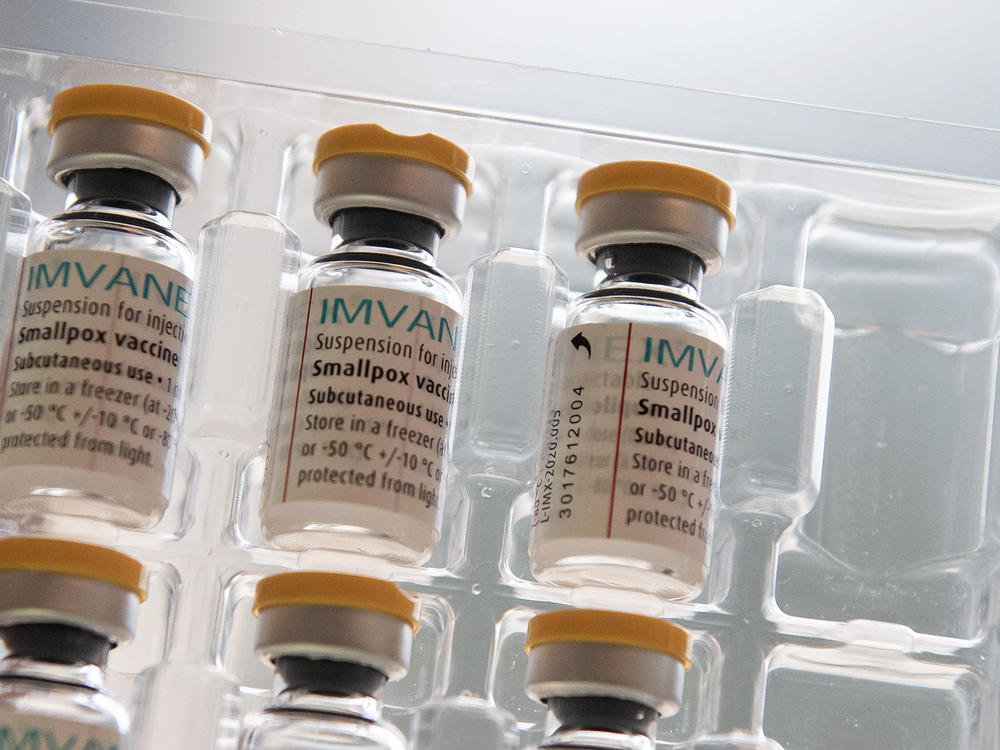
Vaccines have been used to combat mpox outbreaks in other places, including the U.S., Europe and Japan. So far, they have not been approved for use in most African nations.
One challenge is that there is very limited data on how the vaccines work in children – who represent the majority of mpox cases in the DRC – and also minimal data on its use in populations that deal with other health issues, like malnutrition. In March, the WHO's vaccine advisory committee recommended the off-label use of the mpox vaccine in children but urged further study.
There are also major logistical challenges to rolling out an mpox vaccination effort, given that most of the cases are in remote areas and parts of the country face violent unrest. Now that the DRC has declared its intent to use two types of mpox vaccines, its National Regulatory Authority is meeting for a vaccine assessment. While mpox vaccines are likely months away, these steps are being heralded as progress – as is the country's acknowledgement of the scale of the concern.
Should an emergency be declared?
"This situation constitutes a public health emergency," said Samuel-Roger Kamb, the Minister of Health in the DRC, speaking in French at the Africa CDC meeting's closing ceremony. "The Democratic Republic of Congo remains very concerned by the scale and severity of the mpox epidemic which is raging in 23 of the country's 26 provinces."
Nicaise Ndembi, a virologist and senior adviser to the director-general of the Africa CDC, says that, so far, that speech has not been followed by an official declaration of a health emergency. "Meetings are meetings, right? Except if we really take action," he tells NPR.
Ndembi says there are a lot of considerations that come into play before an official declaration can be issued. Many countries vividly – and bitterly – remember how travelers from numerous African countries were banned after Botswana and South Africa shared news about the discovery of Omicron, which was then a new strain of COVID. These bans cost the countries economically and drew criticism since simultaneous cases in Europe did not receive the same response. "So, it's very sensitive," he says.
Nonetheless, Ndembi says his instinct is that the scientific evidence merits a health emergency, particularly because the DRC borders nine countries and the virus could spread through travelers as it did in 2022.
"I would say: Declare! Because, by declaring, you have access to the drugs, you have access to the vaccines. We don't need to go through all the approval processes. And that will open the door for international support to mobilize resources," he says.
But in the interim, there are steps that can be taken, including disease surveillance, emergency response communication, infection prevention control and improved clinical care, even without mpox treatments in the country, says Dr. Rosamund Lewis, the WHO's technical lead and emergency manager for mpox.
"Small children [with mpox] can become dehydrated very quickly. When you have enlarged lymph nodes in the neck and sores in the mouth, children can't eat or drink. So without access to rehydration methods, nasogastric tubes, intravenous [fluids] if needed – without basic medical care that you would take for granted anywhere else – the children have a very high risk of severe disease and death, which we're seeing in the data," explains Lewis.
"Our responsibility, as a global community, is to support and accompany the DRC in their actions," she says.
"I will remind everyone that in two and a half, three years of mpox response, there hasn't been a single penny of donor money invested at a global level for controlling mpox," adds Dr. Michael Ryan, executive director of the WHO's Health Emergencies Programme. "So while the concerns of the world are very well known, I don't see the concerns of the world reflected in the investment of resources needed to actually contain this virus."